
Monthly Archives: January 2018
Dr. Zhang’s Key Tips for Getting Pregnant in the New Year

 If you are having difficulty getting pregnant, you can increase your odds this New Year by being more proactive. Here’s the deal: You must implement a simple plan of action to boost your chances of pregnancy success this New Year.
If you are having difficulty getting pregnant, you can increase your odds this New Year by being more proactive. Here’s the deal: You must implement a simple plan of action to boost your chances of pregnancy success this New Year.
Simple Plan of Action
- Step 1: Schedule your initial consultation with a fertility specialist
- Step 2: Discover why you are having trouble getting pregnant
- Step 3: Implement a customized fertility treatment plan of action
Schedule an Initial Consultation
To avoid any medical complications preventing you from conceiving this New Year, make an appointment with a fertility specialist for a thorough reproductive examination and preliminary evaluation. It can’t be emphasized enough – up to 34 percent of infertility cases are due to structural issues with a woman’s reproductive system. At New Hope Fertility Center, both men and women undergo a complete fertility assessment to evaluate their reproductive health.
Why does this matter? Flagging any potential cause of infertility is the only way to quickly and cost-effectively help you get pregnant this New Year. Once the cause of infertility is identified, a customized treatment plan will be designed based on your medical and personal needs.Read more: Dr. Zhang’s Key Tips for Getting Pregnant in the New Year
A Guide to Your Fertility Preservation Options
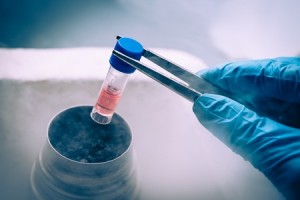 Fertility preservation is the process of saving a person’s physical capability to have biological children in the future. Look: Men and women must know all options available for preserving their fertility for future family planning. Freeze now and preserve your fertility for the future. Here’s the deal: You must locate a fertility preservation center having earned a world renowned reputation as a pioneer in the field of fertility preservation.
Fertility preservation is the process of saving a person’s physical capability to have biological children in the future. Look: Men and women must know all options available for preserving their fertility for future family planning. Freeze now and preserve your fertility for the future. Here’s the deal: You must locate a fertility preservation center having earned a world renowned reputation as a pioneer in the field of fertility preservation.
Division of Fertility Preservation
Our Division of Fertility Preservation provides all-encompassing in cryopreservation technology.
- Egg Freezing – Oocyte Cryopreservation
- Embryo Freezing and the Frozen Embryo Transfer (FET) process
- Ovarian Tissue Freezing
- Sperm Freezing
With over 400 live births from cryopreservation technology, our Division’s mission continues to ensure that everyone has a pathway to family planning – regardless of their life circumstance. We provide the most comprehensive, cutting-edge, and reliable 21st Century solutions for fertility preservation.
Fertility Preservation in Cases of Cancer
New Hope Fertility Center is a world renowned provider of egg freezing treatment for women diagnosed with ovarian cancer. We have partnered with Fertility Preservation – an organization founded by leading onco-fertility specialist – Dr. Kutluk Oktay.
We are one of the world’s leading providers of:
- Ovarian Tissue Freezing
- Ovarian Transplants
- Ovarian Stimulation for Cancer Patients
- Fertility Preservation for Children Diagnosed With Cancer and Turner Syndrome
Identifying Quality Embryos is Key to a Successful IVF Pregnancy
 Quality embryo identification is key to conceiving a successful pregnancy through IVF. Why does this matter? Only quality embryos are transferred during a fresh cycle or cryopreserved for future Frozen Embryo Transfer (FET) procedures. We give careful attention to nurturing and identifying quality embryos as they grow and develop in vitro. Bottom Line: Our embryologists utilize state-of-the-art technology to identify quality embryos.
Quality embryo identification is key to conceiving a successful pregnancy through IVF. Why does this matter? Only quality embryos are transferred during a fresh cycle or cryopreserved for future Frozen Embryo Transfer (FET) procedures. We give careful attention to nurturing and identifying quality embryos as they grow and develop in vitro. Bottom Line: Our embryologists utilize state-of-the-art technology to identify quality embryos.
- EmbryoScope technology
- Genetic Testing – PGD/PGS/NGS
Quality Embryo Growth and Development Expertise
From a cell – to a newborn baby – embryology is the branch of biology and medicine focused on the study of an embryo from the point of fertilization through development to the fetus stage. The expertise practice of embryology is key to pregnancy success through IVF technology.
- Assisting in the surgical retrieving of a woman’s eggs
- Performing post-surgical retrieval tests on eggs
- Performing in vitro tests on embryos
- Maintaining patient clinical records
Excess, quality embryos produced during a fresh IVF cycle are cryopreserved for future transfers via FET. Only the highest quality embryos are cryopreserved for the best chances of a future FET pregnancy success.
Quality Embryos and the EmbryoScope
EmbryoScope technology is used to gather time-lapsed data by closely monitoring every embryo’s growth and development without disruption of the in vitro culturing process.
- Quality embryos have the highest chance of implantation
- Quality embryos thrive into a fetus
- Quality embryos have the best chance of achieving a full-term, healthy pregnancy
EmbryoScope is an innovative, cutting edge, time-lapsed photography and software solution. EmbryoScope is technology designed to improve IVF outcomes.
- Quantitative data on an embryo’s early stage of development in vitro
- Objective information on an embryo’s early stage of development in vitro
- Utilizes time-lapsed photography and software
- No need to manipulate embryos within the incubator in vitro
- No need to remove the embryos from the incubator in vitro
Read more: Identifying Quality Embryos is Key to a Successful IVF Pregnancy
How to Prepare for Your Upcoming IVF Treatment
 I encourage my patients to be mentally and physically prepared for their upcoming IVF treatment, regardless of my recommended protocol:
I encourage my patients to be mentally and physically prepared for their upcoming IVF treatment, regardless of my recommended protocol:
Mental and physical readiness can mean all the difference in IVF pregnancy success.
- Eating a well-balanced diet will increase your chances of IVF success. You should begin improving your nutritional habits at least 3 months before your embryo transfer. Good nutrition enhances the health of your reproductive organs and ensures a quality blood supply to the uterus. Why is this important? Good nutritional habits you develop now will be easy to carry over into your pregnancy.
- Take a good quality multi-vitamin and mineral supplement containing vitamins A, B, D, and C complex. Your supplement should include zinc, magnesium, selenium, iron, and co-enzyme Q10 which all play a vital role in fertilization and implantation. That’s not all. Ask your fertility specialist to prescribe a folic acid supplement to fend off neural tube defects such as spina bifida.
- Reduce your alcohol intake because studies show that women over 30 who drank seven or more alcoholic beverages a week were twice as likely not to conceive. Cutting out alcohol altogether while you try for a baby is the best plan because, once you conceive, your cravings for a drink will be diminished. If you don’t abstain completely from alcohol, opt for only three glasses of red wine per week – sorry, no chardonnay.
- Watch your BMI and get good sleep. A healthy adult Body Mass Index (BMI) is between 18.5 and 24.9. A 2016 review of studies shows that not getting enough sleep leads women to consume an average of 385 more calories the next day. Too much body weight can make women less fertile. Seek help from a dietician and an exercise coach to help you lose weight and maintain a healthy BMI while you are trying to get pregnant. Remember: Your revamped diet and physical fitness regimen will help you to have a healthy pregnancy and baby.
- Avoid Caffeine in coffee, tea, and soda because it can have an adverse effect on female fertility. It’s best to cut caffeine out altogether to boost your fertility level and prepare for a healthy pregnancy. Drinking more than 300 mg of caffeine per day – 2 to 3 cups of coffee – has been linked to a higher risk of miscarriage and stillbirth.
- Exercise increases blood flow to a woman’s reproductive organs and brings in fresh blood to cells. Exercise helps to oxygenate the blood. New studies have shown that both online yoga and in-person yoga help to increase the chances of a successful IVF pregnancy by up to 26 percent. This is because yoga is proven to reduce stress and anxiety in IVF patients. Fertility Yoga regimens include a series of poses and postures designed to improve fertility.
- Acupuncture for Fertility has been proven by studies to increase a woman’s chances of getting pregnant by up to 50 percent! National Institutes of Health research has shown a direct correlation between acupuncture and pregnancy. New Hope Fertility Center has recently launched an in-house acupuncture service as an integral part of our all-encompassing infertility treatment options.
IVF Treatment Doctor
To schedule your initial consultation with Dr. John Zhang at New Hope Fertility Center, click the icon below – or – call 917.525.5496.
How Sleep Increases Fertility
 I recommend women in their prime childbearing years (25 to 35) get 7 to 9 hours of quality sleep every night during a work week. The National Sleep Foundation has found through studies that sleep has a powerful influence on a woman’s reproductive hormonal system.
I recommend women in their prime childbearing years (25 to 35) get 7 to 9 hours of quality sleep every night during a work week. The National Sleep Foundation has found through studies that sleep has a powerful influence on a woman’s reproductive hormonal system.
Sleep Deprivation: BMI – Mood – Stress
Sleep deprivation adversely affects your BMI, your mood, and your stress level. Your Follicle Stimulating Hormone (FSH) level is directly affected by lack of sleep. Your FSH level should ideally be at its highest level just before you ovulate.
Women averaging 7 to 9 hours of sleep each night had a 20 percent higher FSH level than those who go 6 or fewer hours – regardless of age, BMI, mood, or stress level.
Sleep and BMI
A healthy adult Body Mass Index (BMI) is between 18.5 and 24.9. Look: A 2016 review of studies shows that not getting enough sleep leads women to consume an average of 385 more calories the next day.
Here’s the real story about women who don’t get enough sleep.
- They gain weight
- The make less healthy food choices
- They eat foods higher in fat
- They eat low protein foods
Over a five year period, women can gain 2.1 BMI points for every hour of sleep they lose. Why is this important? A two pound weight gain can easily throw a woman off of her healthy BMI.
The takeaway. Sleep is an important moderator of neuroendocrine function and glucose metabolism. Sleep loss alters metabolic and endocrine alterations.Read more: How Sleep Increases Fertility
How ICSI Technology Enhances IVF Egg Fertilization
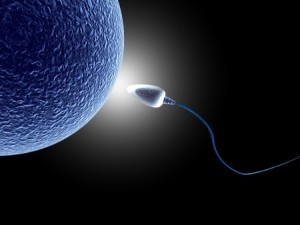 ICSI – Intracytoplasmic Sperm Injection – is a specialized egg fertilization technique used during the IVF process. Look: ICSI bypasses a number of common reproductive conditions preventing sperm from fertilizing an egg. A single sperm cell is injected directly into an egg under the guidance of a microscope. ICSI has revolutionized the treatment of male-factor infertility.
ICSI – Intracytoplasmic Sperm Injection – is a specialized egg fertilization technique used during the IVF process. Look: ICSI bypasses a number of common reproductive conditions preventing sperm from fertilizing an egg. A single sperm cell is injected directly into an egg under the guidance of a microscope. ICSI has revolutionized the treatment of male-factor infertility.
Why is ICSI important?
- ICSI is used to maximize the rate of egg fertilization
- ICSI lessens the chances of sperm not being able to penetrate the wall of the egg
ICSI is recommended for most couples undergoing IVF – especially these candidates:
- Unexplained infertility – known as idiopathic infertility – when the cause cannot be pinpointed
- Male-factor infertility – a man’s sperm is not able to fertilize a woman’s egg
- Combined female- and male-factor infertility
Today, ICSI is routinely recommended to improve fertilization in all IVF cases – regardless of diagnosis.
Sperm Retrieval for ICSI
When a man has a low sperm count and/or motility, a semen sample is collected through masturbation. The semen sample is processed in a special solution to obtain optimum ICSI results.
When a man is suffering from azoospermia – no sperm in ejaculate – sperm is microsurgically retrieved from the testicle or epididymis. This is commonly known as testicular sperm retrieval. Microsurgery to remove sperm from the testicles or epididymis can be performed under local or general anesthesia and requires short recovery periods.
Obstructive Azoospermia (no sperm in semen) can be corrected by the surgical removal of sperm directly from the testis or epididymis of the testicle.
- Microsurgical Epididymal Sperm Aspiration (MESA)
- Percutaneous Epididymal Sperm Aspiration (PESE)
- Testicular Sperm Extraction (TESA)
Non-Obstructive Azoospermia (sperm count with impaired sperm) may be caused by hormonal problems, testicular failure, varicocele, or varicose veins in the testicles. Non-Obstructive Azoospermia can be corrected through TESE – testicular sperm extraction. TESE is a surgical technique using fine needle aspiration performed with local anesthesia.Read more: How ICSI Technology Enhances IVF Egg Fertilization
Discover Needle-Free IVF at New Hope Fertility Center
 We are proud to offer our patients a new, simple and convenient IVF treatment protocol. Look: Needle-Free IVF! This revolutionary IVF protocol eliminates the fear, pain, and anxiety many patients experience with needles. Our Needle-Free IVF protocol stimulates a woman’s ovaries into producing multiple egg follicles through the use of oral fertility medications. The best part? Hormone levels are measured through urine and saliva tests during a Needle-Free IVF cycle.
We are proud to offer our patients a new, simple and convenient IVF treatment protocol. Look: Needle-Free IVF! This revolutionary IVF protocol eliminates the fear, pain, and anxiety many patients experience with needles. Our Needle-Free IVF protocol stimulates a woman’s ovaries into producing multiple egg follicles through the use of oral fertility medications. The best part? Hormone levels are measured through urine and saliva tests during a Needle-Free IVF cycle.
Needle-Free IVF Benefits
Through Needle-Free IVF, patients are able to administer hormone stimulation in a less-invasive manner.
- No shots
- No needles
- No injections
- No blood draws
Needle-Free IVF Protocol
Why Needle-Free IVF is patient-friendly.
- Improves patient safety
- Improves patient compliance with medication regimen
- Reduces possibility of error in medication administration
- Eliminates the risk of accidental needle sticks
Needle-Free IVF Fertility Medications
Depending on the woman’s medical needs, an oral fertility medication – typically Clomid – is prescribed to gently stimulate her ovaries into producing multiple eggs. Synarel is delivered nasally 36 hours prior to surgical egg retrieval.
- Clomid or Femara to stimulate egg production
- Synarel to trigger ovulation
- Oral progesterone tablets
- Vaginal progesterone suppositories
Read more: Discover Needle-Free IVF at New Hope Fertility Center
How In Vitro Maturation (IVF/M) Helps to Increase IVF Pregnancy Success Rates
 IVF in conjunction with egg maturation in a laboratory setting (IVF/M) increases a woman’s chances of using at least some of her immature eggs for in vitro fertilization and transfer. Look: Through In Vitro Maturation (IVF/M or IVM) technology, Dr. John Zhang is able to retrieve and bring some of your immature eggs to maturation in vitro. Why does this make a difference? Typically in past conventional IVF procedures, only mature eggs were surgically retrieved to be fertilized in vitro.
IVF in conjunction with egg maturation in a laboratory setting (IVF/M) increases a woman’s chances of using at least some of her immature eggs for in vitro fertilization and transfer. Look: Through In Vitro Maturation (IVF/M or IVM) technology, Dr. John Zhang is able to retrieve and bring some of your immature eggs to maturation in vitro. Why does this make a difference? Typically in past conventional IVF procedures, only mature eggs were surgically retrieved to be fertilized in vitro.
IVF/M
A Conventional IVF procedure requires a woman to undergo multiple hormone injections to help produce 10 to 15 egg follicles as they reach maturity while they are still in her ovaries. In addition, the patient must endure multiple, regular ultrasounds and blood tests during a one month fresh IVF cycle.
The IVF/M procedure matures a woman’s eggs in vitro – in the laboratory – after they have been surgically retrieved in an immature stage. Here’s the deal: IVF/M requires fewer fertility medications and only a couple of ultrasound and blood tests during a typical one month cycle.
IVF/M cycle fertility medications are typically available in pill and suppository form. The best part? Because fertility medications are scaled back through the IVF/M process, the patient’s cost is reduced.Read more: How In Vitro Maturation (IVF/M) Helps to Increase IVF Pregnancy Success Rates
How AMH Plays a Key Role in Predicting a Woman’s Fertility
 Measuring a woman’s AMH level – Anti-Mullerian Hormone – is crucial to achieving a successful pregnancy through a fresh IVF transfer, as well as for an optimal egg freezing cycle. Why does this matter? AMH testing measure a woman’s ovarian reserve. A woman’s ovarian reserve determines the chances for conceiving and giving birth to a healthy baby using her own eggs. That’s not all. A recent study has found that fertile women having a low AMH level became pregnant less frequently than those with a higher AMH level.
Measuring a woman’s AMH level – Anti-Mullerian Hormone – is crucial to achieving a successful pregnancy through a fresh IVF transfer, as well as for an optimal egg freezing cycle. Why does this matter? AMH testing measure a woman’s ovarian reserve. A woman’s ovarian reserve determines the chances for conceiving and giving birth to a healthy baby using her own eggs. That’s not all. A recent study has found that fertile women having a low AMH level became pregnant less frequently than those with a higher AMH level.
A Woman’s AMH Level Decreases With Age
As a woman ages – post-35 – the count of her egg follicle (ovarian) reserve decreases. Did you know? Obese women have low AMH levels and poor ovarian reserves.
Bottom Line: As shown in the chart below, older women have lower AMH levels than their younger counterparts.
Age 10th Percentile 50th Percentile
18 – 24 1.10 3.60
25 – 29 1.10 3.20
30 – 34 .52 2.10
35 – 39 .20 1.50
40 – 41 .10 .80
42 + .09 .50
Because women with lower AMH levels have less of an ovarian reserve than women with high AMH levels, AMH testing is key to predicting how a woman will respond to fertility medications. Here’s the deal: AMH testing helps Dr. Zhang predict your fertility level – that is – your chances of a successful pregnancy.
Women having low AMH levels do not respond well to fertility medications. These women are classified as poor responders because their bodies to not produce a sufficient number of high quality eggs using fertility medications.Read more: How AMH Plays a Key Role in Predicting a Woman’s Fertility